Army.mil: Excellent Report of How a MEDEVAC Mission Can Run
Medical professionals in Afghanistan strive to treated wounded within ‘golden hour’
June 22, 2011
By Navy Lt.j.g. Haraz Ghanbari

Pfc. Shawn Williams of the 1st Stryker Brigade Combat Team, 25th Infantry Division based in Fort Wainwright, Alaska, is taken to a Black Hawk helicopter for evacuation after being injured by a roadside bomb, Friday, June 17, 2011, in the Kandahar...
KANDAHAR AIRFIELD, Afghanistan, June 22, 2011 — An air ambulance crew from Company C, 1st Battalion, 52nd Aviation Regiment, just finished their lunch in a small break room in southern Afghanistan when a nine-line medical evacuation, or medevac, request was received.
The time was 1:51 p.m., and within a matter of seconds the Soldiers, who are deployed from Fort Wainwright, Alaska, ran a couple of hundred yards to two Black Hawk helicopters.
As the co-pilot and crew chief prepared their helicopter for the critical mission, the pilot and medic were inside the tactical operation center getting grid coordinates and information on the patient. Another couple of minutes passed, and the pilot and medic headed to the helicopter to suit up.
Roughly 10 minutes lapsed since the initial request was received, and the helicopters were now airborne en route to Sha Wali Kot.
Pfc. Shawn Williams, 1st Stryker Brigade Combat Team, 25th Infantry Division, also based in Fort Wainwright, was driving a Stryker vehicle when a roadside bomb detonated and ignited the vehicle on fire. Williams’ foot was fractured, his face covered with hot grease, his right and left hands suffered second-degree burns and were blistering.
As flames engulfed the Stryker and thick black smoke filled the blue Afghan sky, Williams’ battle buddies stabilized him, wrapping his right hand in gauze and providing support to his right foot, while relaying information to the incoming medical evacuation crew. Two Kiowa Warrior helicopters circled overhead providing firepower and checking for additional enemy threats as the medevac pilots made a final approach to the landing zone.
“At the POI [point of injury], the first thing I was concerned about was the security of the pick-up location. Secondary IEDs [improvised explosive devices] targeting the medevac helicopter are a very real threat for us, so we are always looking below and around the helicopter,” explained Sgt. Daniel Sherwin, the onboard flight medic. “A captain approached me and briefly told me the injuries of the patients, and their medic gave me a quick run down of the treatment.”
The nine-line medevac request only noted one patient, but Sherwin learned after landing that another Soldier sustained a possible traumatic brain injury.
Four Stryker Soldiers carried Williams on a litter toward the helicopter, its blades still turning as it sat within eyesight of the damaged Stryker — ammunition exploding inside from the intense heat. Sherwin, a Canadian citizen who has been in the U.S. Army for seven years and is on his second combat tour, walked alongside Williams doing an initial assessment of the patient.
Almost 20 yards from the door of the helicopter, Williams, raising his left hand — blackened from grease — gave his unit the thumbs-up.
Once loaded into the helicopter, the pilots lifted off quickly over the hills and mountains as Sherwin began a more complete evaluation. From head to toe, he checked Williams’ injuries — making sure his airway was clear, he was breathing OK and that he wasn’t bleeding.
“We got the guys loaded as quickly as possible and took off,” said Sherwin. “One of the biggest things we have to offer is speed, so getting off the ground and on our way to the hospital is essential.”

Pfc. Shawn Williams of the 1st Stryker Brigade Combat Team, 25th Infantry Division, based in Fort Wainwright, Alaska, right, is treated by flight medic Sgt. Daniel Sherwin en route to the Kandahar Airfield NATO Role 3 Multinational Medical Unit for...
Sherwin needed to remove Williams’ improved outer tactical vest, a specially designed piece of equipment used to protect servicemembers from various types of war-zone hazards such as shrapnel and different types of ammunition. The vest and its components, typically weighing between 30 to 35 pounds, is at times cumbersome to remove so Sherwin pulls a lanyard attached to the vest causing it to quickly fall apart into four pieces so the triage can continue.
Williams is a priority patient known as “Category A,” because of the potential for loss of life, limb or eyesight.
“I was very concerned about his airway, because inhalations burns will cause swelling,” said Sherwin. “I looked in his nose and mouth to see if there were any signs of burns, and was relieved to not see any.”
Cutting off Williams’ combat shirt and pant legs, Sherwin takes a pulse and starts an IV while monitoring other vital signs.
Due to the noise and vibration of the helicopter it can be difficult to monitor a patient’s breathing, but Sherwin says looking at and feeling the rise and fall of the chest works well.
“The second patient was clearly shaken by the incident, but was in stable condition. He was concerned about his buddy,” said Sherwin. “I quickly got some vital signs on him to be sure he was as stable as he appeared to be. Simply giving them a thumbs up and getting one in return is reassuring to both us and the patient.”
Back on Kandahar Airfield, a distinct series of high-pitched tones alerting the medical staff of an inbound “Cat. A,” cuts through the chatter of nurses and doctors tending to patients at the NATO Role 3 Multinational Medical Unit.
Within moments, a small group of hospital corpsman who comprise the emergency vehicle operator course, or EVOC, team quickly gather their protective helmets and goggles as they reach for their pagers to read the short description of the inbound patients’ wounds.
Climbing into the rear of a specially designed humvee ambulance, the head of the afternoon’s EVOC team radios the hospital’s tactical operations center for an update. The ride from the trauma bay to the flight line is short, but long enough to discuss any critical information about the patient.
Sometimes the patient is stabilized, but other times the corpsmen may need to assist with rending continuous medical treatment until a nurse or doctor takes over in the trauma department.
Pulling up to the edge of the flight line, the driver positions the humvee as the helicopter pilot makes a fast approach to the landing zone. The rotor wash is so strong the corpsmen brace themselves against the side of the humvee until the helicopter has landed, a technique they use to prevent from being blown over.
Two by two, the corpsmen carefully move toward the side of the Black Hawk as Sherwin opens the door. Two corpsmen carry the “head” or top of the litter and two carry the “feet” or bottom of the litter.
The time is 2:51 p.m., and Williams and the second patient are loaded into the ambulance, as a hospital corpsman and Sherwin accompany them. The corpsman radios ahead, and roughly 45 seconds later the team unloads Williams, securing him to combat gurney before another team from the trauma department takes over.
The second patient was able to walk inside.
Once inside the trauma bay, Sherwin quickly briefs a team of U.S. Navy doctors, nurses and corpsmen along with medical professionals from other countries who then begin more advanced treatment.
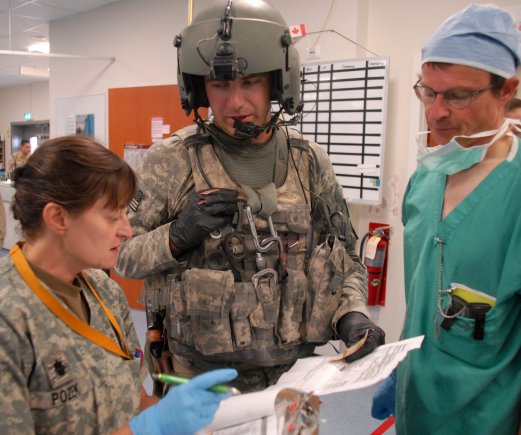
Sgt. Daniel Sherwin of Company C, 1st Battalion, 52nd Aviation Regiment, based in Fort Wainwright, Alaska, briefs members of the Kandahar Airfield NATO Role 3 Multinational Medical Unit's trauma team on the injuries of Pfc. Shawn Williams of the 1st...
“We brief them [the trauma team] on the mechanism of injury, injuries sustained that we have found, all the vital signs, and all the findings in our assessment, to include the status of their bleeding — controlled or not controlled — airway, breathing and the level of consciousness,” explains Sherwin. “Lastly we tell them all the treatments that were done for the patient, and again include what the ground medic did and what we did for the patient in the air — medications administered and the time and dose given is also important for them to know.”
For Williams and his battle buddy, the transfer of care from field medic to flight medic and then to the trauma team occurred within what is known as the “Golden Hour.” Medical professionals have determined that if a critically injured patient receives definitive treatment within 60 minutes from the time of injury, his or her chances for survival increase dramatically.
As part of the transfer of care Sherwin says that all of the information the medevac crew relays is particularly important if the patient is unresponsive, but if the patient is alert and oriented — talking to the doctors and not in any apparent distress — the doctors typically can gather a great deal about the patient’s general condition.
After various tests and treatments, approximately six hours have passed since Williams arrived at the Role 3, and he is recovering in a room with other servicemembers. It’s nearly 9 p.m. and Williams receives a visit by the chief of staff and command sergeant major for International Security Assistance Force Regional Command South and 10th Mountain Division (Light Infantry).
The 21-year-old Soldier, his face now free from grease, his foot better stabilized and his burns beginning to heal, recalls his escape from the burning Stryker and his medevac flight to the hospital.
A 25-year Army veteran, Col. Erik C. Peterson, the chief of staff, requests for the orders to be read awarding Williams the Purple Heart for wounds received in action. As other servicemembers stand at attention, Peterson clips the medal to a white blanket Williams is using to keep warm.
Peterson asks Williams about his family and his unit, and then the three share a few laughs. Prior to departing, Command Sgt. Maj. Christopher Greca, himself a Purple Heart recipient, presents Williams with a command challenge coin.
For the next several hours, Williams rests under the observation of a nurse and corpsman before departing for Landstuhl Regional Medical Center in Germany for additional treatment en route back to the United States. At 4:25 a.m., Williams is discharged from the Role 3 for the next chapter of his recovery.
Stories similar to Williams’ occur everyday at the Role 3 with patients arriving by medevac or sometimes ambulance. Injuries range from debris in a person’s eyes to a servicemember who has suffered a catastrophic injury such as the loss of multiple limbs.
Patients can include coalition servicemembers, Afghan national security forces, local nationals as well as military contractors.
The article can found here.